Breathing is one of the most fundamental functions of the human body, yet how we breath, through the nose or the mouth, can have a profound effect on development, structure, and overall health.
In both children and adults, mouth breathing is often seen as a common pattern, but from a clinical perspective, it is not normal. It is typically a sign that the body has adapted to a challenge within the airway structures (including the sinuses, structural compensations in the cranium or palate, or nervous system dysfunction).
Nasal Breathing is designed to be the primary airway for several important reasons: it filters and humidifies air, it helps regulate oxygen and carbon dioxide balance, it supports nitric oxide production, which improves oxygen delivery, and it promotes proper tongue posture and craniofacial development.
When nasal breathing is functioning well, it supports both structural growth and neurological regulation.
Mouth breathing occurs when a person habitually breathes through the mouth rather than the nose, during sleep, at rest, or with activity, this is not simply a habit. It is a compensatory pattern, meaning: the body is choosing the easiest available airway based on its current structure and function.
Mouth breathing can result from a combination of structural, neurological, and environmental factors, including:
- Narrow or underdeveloped maxilla (upper jaw)
- High, narrow palate reducing nasal airway space
- Cranial distortions affecting nasal passages
- Cervical spine restrictions influencing airway tone
- Dural tension patterns impacting cranial base function
- Enlarged tonsils or adenoids
- Allergies or chronic congestion
In many children, these patterns begin with birth stress or early cranial distortion, which then influences airway development over time.
When mouth breathing occurs during development, it can influence:
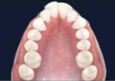
1. Craniofacial Growth
- Narrow palate
- Long, narrow facial pattern
- Dental crowding
- Altered jaw development
2. Feeding and Oral Function
- Poor tongue posture
- Difficulty with latch (in infants)
- Swallowing dysfunction
3. Sleep and Behavior
- Restless sleep
- Snoring or sleep-disordered breathing
- Daytime irritability or attention challenges
4. Nervous System Regulation
- Chronic airway stress can influence autonomic balance and the child’s ability to regulate.
In children, mouth breathing is rarely beneficial. The only “advantage” is that it allows immediate compensation when nasal breathing is restricted
However, this should be seen as a short-term adaptation, not a healthy long-term strategy.
In adults, chronic mouth breathing may contribute to:
- Poor sleep quality
- Snoring and sleep apnea
- Dry mouth and increased dental issues
- Reduced oxygen efficiency
- Fatigue and decreased performance
It may also reflect long-standing structural patterns that began in childhood.
In certain situations, with adults, mouth breathing can be useful: during intense physical exertion when oxygen demand is high, and when nasal passages are temporarily blocked.
Airway Function: The Central Issue
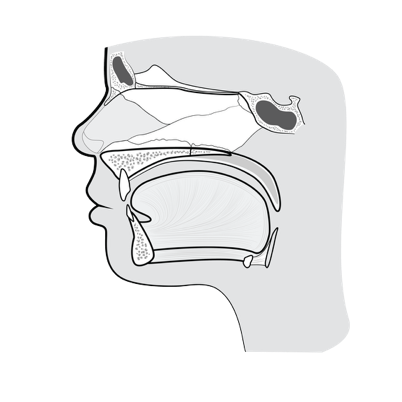
At the core of mouth breathing is airway function.
The airway is not just a passive tube it is influenced by:
- Cranial structure and the cranial facial bone relationships (frontal, maxilla, sphenoid, nasal bones)
- Palate shape and size
- Tongue position
- Cervical spine alignment
- Dural membrane tension
- Neurological control of breathing
The airway reflects the integration of structure and neurological function. When any part of this system is compromised, the body adapts, and mouth breathing often becomes the solution.
The Chiropractic Perspective
The goal is not simply to “stop mouth breathing,” but to identify and correct the underlying pattern
Evaluation includes:
- Cranial assessment (sutures, fontanelles, primary and secondary respiratory mechanics, boney structure, etc.)
- Cervical spine (especially Occiput–C1–C2)
- Dural and fascial system tension
- Tongue posture and oral function (nursing, swallowing, chewing, etc.)
- TMJ (jaw function and mechanics)
- Breathing pattern observation
Chiropractic care should focus on restoring balance and function to the underlying structures and neurology involved including but not limited to:
- Cranial Adjusting Corrections
- Cervical Spine Evaluation and Adjustments
- Dural Tension Balancing
- Cerebrospinal Fluid Mechanics (the lymphatic system of the central nervous system)
- Sinus congestion issues (chronic inflammation, allergies, structural deviations or restrictions)
Supporting Change at Home
Parents and patients can support airway function by:
- Encouraging nasal breathing during the day
- Promoting proper tongue posture (on the palate)
- Supporting tummy time and movement in infants
- Addressing sleep positioning
- Seeking collaborative care (ENT, Allergist, myofunctional therapy when appropriate)
Mouth breathing is not the problem it is the body’s solution. The real question is, why is the body choosing that solution?
Mouth breathing is common in both children and adults, but it is often a sign that something deeper is influencing airway function and development. By recognizing it early, understanding its causes, and addressing the underlying structural and neurological patterns, we can support improved outcomes both short and long-term. It is about helping the body return to a state of balance, adaptability, and optimal function.




